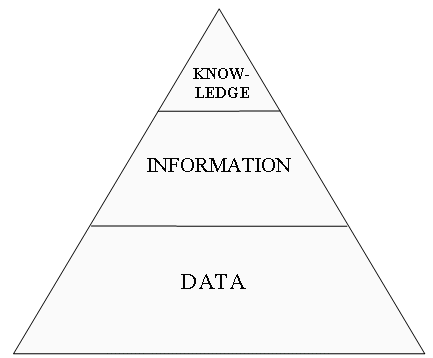
Fig. 1. “Medical informatics pyramid”.
Data are on the lowest level of the
hierarchy; they consist of some “primary facts” (“Patient N’s blood
pressure is 120/70 mm Hg”).
Information is usually some data or data arrays within a context (“At 9 am patient N’s blood pressure was 120/70 mm Hg, patient M’s blood pressure was 150/100 mm Hg”).
Knowledge is a usually derived from significant amount of information. As a rule, knowledge tends to lead to some practical application (“Salt consumption should be restricted to decrease the risk of hypertension”.
More detailed hierarchy of data flow was suggested by R. Gibson Parrish and S. M. McDonnel [3] (see Fig. 2).
Overall, both examples of data flow are very similar; however, the second figure includes two additional items: the primary event and the response action (both items are really outside the health informatics system). The societal problems usually occur at the levels of registration of the events and dissemination/use of information. It can easily be explained: medical informatics is rather a subsystem within health care system, to serve its needs. For the whole society the system providing necessary health data flow usually remains a kind of “black box”. Therefore, societal effects may appear rather in the process of healthcare information input and output.

Fig. 2. Medical data flow from primary event to response.
Information is usually some data or data arrays within a context (“At 9 am patient N’s blood pressure was 120/70 mm Hg, patient M’s blood pressure was 150/100 mm Hg”).
Knowledge is a usually derived from significant amount of information. As a rule, knowledge tends to lead to some practical application (“Salt consumption should be restricted to decrease the risk of hypertension”.
More detailed hierarchy of data flow was suggested by R. Gibson Parrish and S. M. McDonnel [3] (see Fig. 2).
Overall, both examples of data flow are very similar; however, the second figure includes two additional items: the primary event and the response action (both items are really outside the health informatics system). The societal problems usually occur at the levels of registration of the events and dissemination/use of information. It can easily be explained: medical informatics is rather a subsystem within health care system, to serve its needs. For the whole society the system providing necessary health data flow usually remains a kind of “black box”. Therefore, societal effects may appear rather in the process of healthcare information input and output.

Fig. 2. Medical data flow from primary event to response.
Unfortunately, in Russia not enough
attention has been paid to medical informatics in general, in particular,
to information data flow in occupational and environmental health.
For example, there is no keyword “medical informatics” in the catalogues
of State Central Scientific Medical Library in Moscow, so the search
by this keyword was not possible. The term “medical information” could
only be found in the catalogue of the library for 1970-1990 (nine entries
were available, seven of them before 1975), Alternatives like “expert
systems”, “medical information”, “databases”, or “computers” were also
not available in the library catalogue.
Though searching through MedLine using the above terms identifies a few articles in Russian journals, the number originating from Russia is substantially lower than that found in industrially developed countries. Other former socialist countries have made greater scientific contribution in this area, which can be seen when we compare the relative number of publications per 1000 physicians in the country (see Table 1).
These figures just help to illustrate the lack of development of medical informatics in Russia in occupational and environmental health.
Unreliable data on the extent and scope of Russian occupational health and the lack of information on environmental health limits the ability to accurately prioritize these socially-important areas within the field of public health. Therefore, one can presume that in Russia proper political decisions regarding occupational and environmental health are hardly possible now, due to lack of accurate data and reliable information.
Number of MedLine entries as of July 1, 2002; number of physicians in the countries according to Encyclopedia Britannica 1997.
Though searching through MedLine using the above terms identifies a few articles in Russian journals, the number originating from Russia is substantially lower than that found in industrially developed countries. Other former socialist countries have made greater scientific contribution in this area, which can be seen when we compare the relative number of publications per 1000 physicians in the country (see Table 1).
These figures just help to illustrate the lack of development of medical informatics in Russia in occupational and environmental health.
Unreliable data on the extent and scope of Russian occupational health and the lack of information on environmental health limits the ability to accurately prioritize these socially-important areas within the field of public health. Therefore, one can presume that in Russia proper political decisions regarding occupational and environmental health are hardly possible now, due to lack of accurate data and reliable information.
Table 1.
Number of scientific articles on medical informatics listed in MedLine,
originated from Russia, some European countries and the USA.
|
“Medical informatics” +
“occupational health” |
“Medical informatics” +
“environmental health” |
|||
|
Abs. figures
|
Per 1000 physicians
|
Abs. figures
|
Per 1000 physicians
|
|
|
Russia
|
17
|
0.025
|
14
|
0.022
|
|
Ukraine
|
10
|
0.043
|
2
|
0.008
|
|
Hungary
|
0
|
0.0
|
0
|
0.0
|
|
Poland
|
5
|
0.058
|
0
|
0.0
|
|
Finland
|
5
|
0.384
|
0
|
0.0
|
|
Sweden
|
2
|
0.091
|
2
|
0.091
|
|
Germany
|
8
|
0.030
|
5
|
0.019
|
|
USA
|
144
|
0.215
|
108
|
0.161
|
Number of MedLine entries as of July 1, 2002; number of physicians in the countries according to Encyclopedia Britannica 1997.
3. The importance of occupational and environmental health for society
Adverse health consequences due to
occupational factors (at work) and due to environmental factors
are common in all countries and often lead to significant loss for
national economies (see below the data on US and Russian loss due
to occupational illnesses and injuries). Unlike most non-communicable
diseases (e.g. diabetes, duodenal ulcer, etc.), occupational and,
partially, environmental diseases have more anthropogenic origin. All
occupational illnesses and most of environmental disorders are preventable.
Therefore, the questions of legal responsibility for the emergence
of these diseases are acute. The issues regarding this responsibility
often have strong legal and political implications.
Occupational diseases have been more precisely studied and categorized, than environmental diseases; therefore it is easier to estimate the loss due to occupational diseases. For example, the investigation performed in the USA [4] demonstrated that approximately 862,200 occupationally related illnesses were estimated to occur annually in the civilian American workforce. The total direct ($65 billion) plus indirect ($106 billion) costs were estimated to be $171 billion. Injuries cost $145 billion and illnesses $26 billion. These estimates did not take into account costs associated with pain and suffering, as well as costs associated with in-home care provided by family members. Overall, because of the inadequacy of surveillance of disease the numbers of occupational and illnesses are likely to be underestimated.
Comparatively, the economical burden of AIDS was estimated at $33 billion, $57 billion for Alzheimer’s disease, $164 billion for circulatory diseases, and $171 for cancer.
Unfortunately, no official estimates are currently available for Russia. The rough estimates are derived from the above-mentioned U.S. figures, and are based on the two following assumptions:
1) the economic burden due to occupational illnesses is directly related with national GDP level (reflecting the overall production level of the national economy).
2) the economic burden is associated with the registered numbers of occupational patients per annum.
The ratio of the US GDP/Russia GDP was approximately 20 (for 1994). If we assume that the occupational morbidity in Russia and the USA is roughly similar, Russian economic loss due to occupational illnesses might total $8 billion ($3 billion direct and $5 billion indirect). Still, there is a great difference between the figures of occupational morbidity in the countries: US Bureau of Labor Statistics reported 429,800 new cases of occupational diseases in private industry in 1999 [5]. The Russian Federal Center of State Committee for Sanitary and Epidemiological Control reported 283,851 cases of occupational illnesses in Russian Federation during last 30 years (1972-2001) [11]. If we assume this Russian figure to be correct, we have to assume that the economic burden due to occupational illnesses in Russia is substantially less (45 times) than the calculated estimation of $8 billions – about $170 million. Given that the latest modest figures are reliable, and these figures reflect the actual societal burden correctly, we might agree that little attention is paid by society to the problem of OEH. But only the expenditures of the Russian Fund of Social Insurance in 2000 were 12 billion RUR [6] – approximately $400 mln., or significantly higher than our “optimistic” estimation. The most pessimistic estimate was made by the chief Russian specialist in occupational health, academician N. F. Izmerov, who reported it to be “10-20% of Russian GDP” [7].
Nevertheless, a major question is whether Russian figures of occupational morbidity are reliable. This question will be discussed in more detail below.
The problem of economic burden estimation due to environmental health disorders is even more complicated than the assessment of occupational illness burden, mainly due to the fact that the definition of environmental illness (health disorder) is unclear, or at least not as fully developed as the definition of occupational disease.
WHO stated (draft definition developed at a WHO consultation in Sofia, Bulgaria, 1993): “Environmental health comprises of those aspects of human health, including quality of life, that are determined by physical, chemical, biological, social, and psychosocial factors in the environment. It also refers to the theory and practice of assessing, correcting, controlling, and preventing those factors in the environment that can potentially affect adversely the health of present and future generations”. It should be mentioned that there are at least 27 other definitions of environmental health [8].
It is obvious that a person may inhabit a series of different environments in the course of his life or even in the course of the day. Ambient environments vary by geography and may vary markedly even within a single city.
A broad spectrum of agents has been associated with chronic health effects in the population. For example:
- Ambient air pollutants (ozone, particulate matter, toxic chemicals, etc.)
- Indoor air pollutants (formaldehyde, carbon monoxide, tobacco smoke, etc.)
- Pesticide resides in food (some of them are suspected carcinogens)
- Disinfection byproducts in drinking water.
It is important to note that the relationship between the environment and health status is modified by many factors (e.g., age, sex, genetic makeup, state of health, dietary habits, etc.), so in general, an individual’s health response to environmental factors can be very different. So, a strict legal definition of the term “environmental disease” remains elusive. This dilemma explains the hardship in establishing the connection between environmental factors influence and resulting health disorders. Often the direct relationship for a single individual cannot be found, and in such cases, the relationship may be revealed only using statistical methods.
Currently, we live in an age of environmental alertness. The social (and political) importance of environmental health cannot be overestimated. Environmental health impacts a wide strata of the population, or rather, the population at large (i.e., if we discuss the problem of ambient air pollution). At the same time, occupational health is actually only a small part of environmental health, as the occupational environment is just a small part of the environment as a whole.
The issues regarding responsibility for health disorders due to environmental factors (especially, anthropogenic environment pollution) can be seen as very acute; especially now, when attention of society has been largely focused on environmental issues. There is a fragile balance that exists between the interests of industry and the interests of the population exposed to the industrial pollutants. The balance of the interests should be established mainly by political processes.
There are two main types of primary data in occupational health – the data regarding work conditions of an individual worker and the data which focuses on his/her health status. In Russia, the data on work conditions (the hygienic characteristics of workplace) are collected by local centers of sanitary and epidemiological control. The person responsible is usually an industrial hygienist, who may either use the available data on working conditions at the specific enterprise, or conduct a workplace evaluation (e.g., measure ambient air in a workplace for concentrations of chemical substances). The data on working conditions are presented to the occupational physician, to whom the worker is referred. The occupational physician, usually in a Regional/Republican Center of Occupational Pathology, compares clinical findings and medical records of the patient with the industrial hygiene data. Then, a determination is made by a commission of the Center of Occupational Pathology (according to the proper normative documents issued by the Healthcare Ministry of Russian Federation) whether a person has or does not have an occupational disease.
Obligatory registration of patients with occupational diseases in Russia was introduced as early as in 1924 [9]. Until 1986, the reports of registered occupational diseases were submitted quarterly by local sanitary and epidemiological stations (later renamed “centers of sanitary and epidemiological control”). Since 1986, individual registration of new cases of occupational diseases began, not just number of cases for each enterprise or territory. The system of registration was automated, which enabled easier analysis of the data. Some regions of Russia introduced more complex computerized systems of registration and analysis of occupational diseases, which were able to perform deeper statistical analysis [9].
According to the Order of Healthcare Ministry of Russian Federation #130 (of 23.06.1994), the system of Centers for Occupational Pathology was created. Previously (during the Soviet years), a system of several Research Institutes of Hygiene had to provide occupational health services for all the Russian workers, but the Institutes were too few and too distant from many of industrial centers to cover the needs in post-Soviet Russia.
Newly created Centers for Occupational Pathology were tasked with creating data banks on occupational morbidity, mortality, and disability. Nevertheless, at some territories the new Centers were not created (e.g., Vladimir region), and some regions’ “Centers” consisted of no more than 2-3 physicians, and were not real centers in the full sense of the word (e.g., there was a single occupational physician working part-time in Mari El Republic with population of 750,000).
Virtually, now there are several parallel systems of registration of occupational diseases functioning in Russia:
1) within the system of Centers for Occupational Pathology (led at the federal level by the Research Institute of Labor Medicine of Russian Academy of Medical Sciences) – the origin of primary data;
2) within the system of the Centers for State Sanitary and Epidemiological Control (led by the Federal Center);
3) within the Ministry of Labor and Social Security;
4) in the Fund of Social Insurance against Occupational Injures and Diseases
The need for the integrated Registry of Occupational Diseases was discussed in Russia for several years, but the creation of the Registry is still in the process.
Beginning in 2001, the first approaches toward the creation of the Registry were published. According to the published data [11], The State Registry of Occupational Diseases in the Russian Federation should be “a system for active dynamic surveillance over the patients with registered occupational disorders in order to:
1) preserve the worker’s health and capacity to work ;
2) provide full compensation of health impairment or disability;
3) minimize the causes for occupational disorders;
4) develop and implement economically feasible mechanisms for improvement of working conditions;
5) develop and implement the state policy toward preservation of workers’ health”.
Unfortunately, until now, the occupational statistics are limited only to the registration of new cases of occupational diseases. Summary statistics are not available yet, which prevents not only estimation of total national burden due to occupational disorders, but also prevents follow-up of occupational cases (if it results in disability or not, etc.). Currently, the newly created Fund of Social Insurance against Occupational Injuries and Diseases has surveillance data only on a portion of occupational patients, those who have been compensated. Still, this system only reaches a part of all occupational patients. The workers who just leave their workplaces due to occupational diseases, but do not receive any material compensation, miss the records of Fund of Social Insurance.
In general, several problems are well-known, preventing adequate surveillance of occupational cases in most countries:
- employers are not interested reporting of occupational cases (even if compensation to workers with occupational diseases is not paid directly by them, higher figures of occupational morbidity at the individual enterprise may result in higher employers’ payments to the social security institutions);
- employees are also not always interested in reporting of work related illness or injury (official registration of disease might mean leaving a rather lucrative job and may also create a hardship in searching for a new job).
In Russia, some additional negative factors may also be present:
- There was a tradition of unreliable statistics during Soviet times. (Until Perestroika, the official figures of occupational morbidity had to be decreased year by year, despite whatever reality existed, to prove the “superiority” of the socialist system. A demonstrative example can be illustrated with a situation at a chemical plant in Nizhny Novgorod region, where all cases of contact eczema were registered as “viral respiratory disorders” – so that the workers could leave work connected with handling allergens for several days without “worsening” local occupational statistics.
- Currently, a “black-market economy” forms a significant part of the Russian economy (according to some estimates, up to 40%), so a portion of workers are considered to be unemployed, but actually, they are employed at some black-market enterprise, where they might be handling some hazardous factors. Surely, such workers would never be eligible for any compensation in case of their disease or injury, and no occupational health statistics is available for this significantly large group of workers in Russia.
- A rather low level of monetary compensation for cases of occupational disorders may keep workers from applying although, on the other hand, excessive compensation might inflate the actual number of occupationally diseased workers).
- The number of physicians allowed to diagnose occupational disease is insufficient (in Russia, only occupational physicians working in Centers for Occupational Pathology are allowed to make diagnosis of occupational disease, and the number of such physicians is less than 1,000, while in the US, there are at least 2,400 physicians certified in occupational medicine [5]).
- Few workers possess the knowledge to wade through the bureaucracy of the occupational insurance and compensation system in Russia, often they are not aware of their rights, and sometimes they might be mislead by their administration (very little attention is paid to occupational topics by mass media, including newspapers, television, and Internet sites).
The latest available figures of occupational morbidity in Russia seem to be too low to be correct – 2.24 per 10,000 employees (official data for 2001 [11, 12]).
At the same time in the USA, this figure was 49.8 illnesses per 10,000 full-time workers [13], a 22-fold increase compared to Russia. This increase cannot be explained by better working conditions in Russia – officially, up to 25% of all working places in Russia do not comply with industrial hygiene requirements [12]. The differences might be slightly less dramatic, when one takes into account that the US index is calculated per 10,000 full-time workers, while Russian index is calculated per 10,000 total workers, and the number of part-time workers at current economic conditions of Russia is substantial.
A scientific assessment should be performed in Russia to capture a more reliable and accurate occupational morbidity, which according to rough estimates, should be considered at least at the level of other industrially developed countries (e.g., the USA), but may even exceed the figures reported in Western countries. As occupational mortality in the USA is about 4 times less than the index found in Russia, we should expect a similar ratio between occupational morbidity – or, approximately, a 90-fold underreporting of occupational diseases in Russia.
It is interesting to compare the registration of occupational morbidity with the registration of intrahospital infections in Russia. There has been usual controversy regarding the official statistics of intrahospital infections as well. Recently The Chief Sanitary Physician of Russian Federation, G. G. Onishchenko, in his Decree #37 (of 06.11.2002), in reference to the data found in the investigation of the registered number of intrahospital infections), stated that the official number was approximately 50 times less than the real number. His decree was an honest attempt to try to correct what he saw was a blatant underestimation of the scope of disease, although it disputed the officially sanctioned statistical data.
The analysis of occupational health information is mainly a comparison of working condition data and workers’ health data. Being compared, the data provides healthcare professionals with information on occupational risks.
The following definition of the term “occupational risk” is given by Federal Law “On obligatory social insurance against occupational injuries and diseases”: “The occupational risk is the probability of a health disorder (loss) or death, connected with carrying out the duties according to labor contract (or in other cases, stated by law)”.
Speaking of occupational risks evaluation, it should be mentioned that the first computerized systems for this were created in 1970s. The Latvian system KASMON was introduced at the USSR level in 1980s. The “occupational health unit” was available for KASMON system, written in BASIC. Now more up-to date computerized systems are used in Russian occupational health. At the moment, the Research Institute of Labor Medicine (in Moscow) prepares “The handbook on occupational risk assessment”. In this handbook the issues of occupational risk due to noise, vibration, dust and some other hazardous factors will be covered [9].
The evaluation of occupational risks is very popular now in Russian medical science. During 2002, 18 Russian articles covering the topic of occupational risk were quoted by MedLine. The occupationally-related risks of coronary heart disease, arterial hypertension, carcinogenic effects, occupational bronchopulmonary diseases, reproductive disorders, etc. were included.
Though the methodology of occupational risk estimation is well known, there is an opinion that the risk estimation must not be correct if it is based on unreliable occupational morbidity data [15]. Perhaps, this explains a rather skeptical attitude toward the occupational risk estimation methodology. It is clear that if morbidity figures are still unreal, risk estimation based on the figures is also far from being correct, so the practical measures suggested according to the estimations will always be questionable for society.
Meanwhile, currently the occupational risk data are not supposed to be used by Social Insurance Fund to calculate the employers’ dues, only the number of registered occupational diseases is used compared to the number of them during previous year [14].
Unlike in most industrially developed countries, the topic of occupational health is not one that receives much public attention in Russia. This lack of public and media attention can be seen by comparing the number of media stories run on occupational health in leading Russian and American newspapers.
In “Rossiyskaya Gazeta” (“The Russian Newspaper”, one of the most influential and widely circulated newspapers of Russia), from 2001 to March 2003, only 6 articles mentioning the key terms “occupational diseases” were found (no full analogue of the English language term “occupational health” is available in Russian language). At the same time, on the website of “USA Today” 312 entries searched by the terms “occupational health” were found for the same period. In several instances, the articles addressing occupational health topics appeared on the front page of several American newspapers as the “lead stories” (e.g., the article “Court to decide scope of disabilities act” appeared on front page of “USA Today” on 04.17.2001). Such a prominent place rarely, if ever, has occurred regarding an article on occupational health in the Russian press.
It can also be demonstrated that virtually no information on occupation health and safety is available on the websites of the Russian Trade Unions or any of the political parties (including even the left-wing parties).
In summarizing the general impression of today’s state of health informatics within the occupational health system of Russia, we must explicitly state that the system is unsuitable for the current needs of Russian society – it is generally based on old-style Soviet principles, and strongly needs to be up-dated. There are some positive “seeds” in the system, such as the risk assessment methodology, that must be kept; but the system of primary data collection should be restructured. Other measures should also be taken to draw the attention of the Russian society (in particular, the trade unions, journalists, and politicians) to the opportunities that occupational health offers in promoting health and quality of life by preventing and controlling workplace disease, injury, and disability.
In the 1990s, the system of social and hygienic monitoring (SHM) was launched in Russia.
The legal basis for the SHM system originated from the “Statement on Social and Hygienic Monitoring”, which was approved by RF government on June 1, 2000. “The Statement” described SHM as “the state system of surveillance, analysis, estimation and prognosis of the state of population health and human environment”. The same statement established the Federal Information Fund of SHM data as “the repository for data on the state of population health and human environment, which includes information acquired through long-term surveillance, as well as legal documents and reference materials on the analysis, prognosis and relationship between environmental factors and human health.”
The primary data are collected in their entirety: population health indices, social and economical indices, ambient air pollution, drinking water quality. According to Order # 334 of the Healthcare Ministry of Russian Federation (of 27.08.1999), there are two levels of data represented:
- from the local level to the regional level;
- from the regional level to the Federal level.
There is a comprehensive list of the health, social and hygienic indices to be used [16]. The indices provide mainly basic statistical information, whose standard methodologies have been utilized for decades (e.g., mortality indices). There are also data on environmental pollutants from the most widely used chemicals. Because most of such indices are based on standard measurable outcomes (e.g., specific levels of chemicals or number of deaths from specific causes) they may be more accurate and reliable than e.g. occupational morbidity data.
The SHM system inherited the ideas of some previous systems for health effects surveillance. For example, by the end of 1990s the system of birth defects registration was created in Russia (based on several normative documents, including The Order of Healthcare Ministry #268 of 10.09.1998). Unfortunately, initially the data of birth defects were collected in the regions of Russia without any connection with pollution data. Currently the comparisons between environmental pollution and birth defects rate can be performed.
Russian investigators V. M. Cherepov, D. I. Timokhin, O.V. Klepikov, V. V. Zhukova (2000) have emphasized that SHM data should be detailed enough to allow their use in making effective managerial decisions [17]. However, according to the same authors, there are some specific features which might limit the possible use of the SHM system:
- the character of the data and their variability;
- the limitations of the algorithms used for making managerial decisions;
- the technical limitations;
- a time lag between the collection of the data and their analysis and publication;
- a time lag before any intervention evaluation can be performed;
- lack of cost-effectiveness of the informational systems;
- inherent complexities of social and political interpretation of the data.
It should also be mentioned that there is controversy involving the need for the timely flow of information versus the accuracy and reliability that comes with this faster transfer of information. Two approaches have been mentioned – first, whether to limit the raw data at the input level (to prevent the “flood” of data at the higher levels), or second, to allow the passage of the raw data directly to the higher level, which would then provide some data verification and analysis. The first approach would be preferred if the primary level of data collection were made fully reliable, and then at least, partial analysis of the data could be performed at this level.
Usually, the supposition is that the higher levels of organizations or government (regional, Federal) are better equipped and have more qualified personnel to a more thorough analysis of raw data.
Specific software was designed to provide data flow within the SHM system. Perhaps one of the best is the automated system “Social and hygienic monitoring”, developed by “Krista”, a software company of Rybinsk, Yaroslavl region [18]. This is a distributed database, which is able to provide SHM data flow within the whole region (from local districts to regional offices, and finally, to the Federal level), and it fulfills the requirements of the Healthcare Ministry with regards to SHM. It is adaptable to the needs of specific users, and certain features can be added upon users’ request.
Russian medical scientists and authors from other countries have suggested that it would be advantageous if certain environmental data (e.g., air and water pollutants) were collected by automated quantitative sampling devices, so that the data could not be tampered with or falsified by personnel [19, 20].
According to “Statement on Social and Hygienic Monitoring”, the aims of SHM system in Russian Federation are the following:
- to document and assess risk factors able to cause harmful effects on human health;
- to identify, evaluate, assess and predict the state of human health and environment;
- to define urgent and long-term measures for prevention of harmful environmental effects on human health;
- to formulate recommendations on controlling and reduction of exposures, illness, and injury regarding human health and environment
- to disseminate information to state and local authorities, other institutions, and the citizens on the SHM results.
The concept of SHM is based on the principles of environmental risk assessment which were introduced by the Chief State Sanitary Physician of Russian Federation G. G. Onyshchenko and Chief State Inspector for Nature Protection of Russian Federation, A. A. Solovianov (common document of 10.11.1997). It was stated that at the beginning of the work on environmental risk assessment in Russia, the U.S. EPA experience would be widely used, after adjusting for Russian conditions. The project was sponsored by some international organizations, e.g., US Agency for International Development, International Bank for Reconstruction and Development.
The term “risk” as defined was very close to the definition given in the U.S. EPA glossary: “The potential for realization of unwanted, adverse consequences to human life, health, property, or the environment; estimation of risk is usually based on the expected value of the conditional probability of the event occurring times the consequence of the event given that it has occurred” [21].
Using the SHM system information on a regional level, many regions of Russia were able to calculate environmental risks, or were able to compare the environmental risks with other health risks. One of the first regions able to perform such analysis was the Yaroslavl region, where the above mentioned SHM software was introduced [22]. Some interesting data were obtained in Udmurtian Republic [23] on risk factors associated with adverse health effects among the Udmurtian population. For example, it was found that alcohol abuse increased the risk of overall health disorders 3.1 times, smoking increased the risk 2.9 times, environmental pollution increased the risk 1.8 times. In Saratov region, nine main risk factors were identified, associated with the occurrence of overall health disorders in the population [24]:
1) Pesticide-containing food products (18.8%);
2) Air pollution at work (16.4%);
3) Nitrate containing food products (12.8%);
4) Marriage status (11.2%);
5) Air pollution at home (10.7%);
6) Elevated noise levels at home (8.2%);
7) Water pollution (7.6%);
8) Elevated noise levels at working place (5.9%);
9) Poor living conditions (4.7%).
Investigators of the Nizhny Novgorod Research Institute for Hygiene and Occupational Pathology reported on the health status of approximately 1000 newborn infants in one of the main centers of Russian chemical industry, Dzerzhinsk [25]. Children of the mothers handling potentially teratogenic chemicals at work were found to have slightly better performance and health indices than children born from mothers who had never worked in the chemical industry. Although the results seemed unexpected, the differences in income rates offered some explanation. According to these additional data, mothers working in chemical industry had much better salaries than those who never worked with chemicals (teachers, librarians etc.). This example supports the assertion that the data for SHM should be as detailed as possible, and should be analyzed in their entirety, without missing social indices.
Missing the comprehensive nature of the data may result in neglecting some important aspects of human health.
Some examples of the use of existing data based on the SHM system were given above. We suppose that SHM data might be used to rank previously identified risk factors, rather then finding new ones. For example, if we look at the list of potential risk factors provided for Saratov region [24], it can be agreed that all the factors listed were considered to be harmful decades ago. Still, the importance and impact of social factors (e.g., salary rate) upon health outcomes has recently been introduced into the social consciousness in Russia. After many decades of declared “social equality”, it has taken some time for the importance of social factors’ impact on public health to be officially acknowledged.
SHM system is rarely discussed in public; now it seems to remain just a working system inside The Healthcare Ministry of Russian Federation.
Though “The Statement on Social and Hygienic Monitoring” described that one of the aims of the SHM system to be “to inform state and local authorities, other institutions and the citizens on the SHM results”, little information on these results is available, excepting several proceedings of the scientific conferences, published as no more than 1500 copies.
The mass media seldom pays attention to so “dull” a topic; it usually focuses only on events such as large-scale environmental disasters. On the Internet, the most interesting information could be found at the website of the Federal Center of State Sanitary and Epidemiology Control [26], but SHM data are restricted from the public viewing by password protection and is available only to certain healthcare authorities.
The ability of managers to use the SHM system to make improvements in the quality of health care will be the single best criterion in evaluating its effectiveness [17]. Nevertheless, if the ability to use the system is delayed (and part of its utility will necessarily be delayed for decades – e.g., in case of tracing the carcinogenic activity of some identified pollutants) – the efficacy of the system as a whole will remain questionable.
Unfortunately, neither “The Statement on Social and Hygienic Monitoring” nor other government documents delineate how the results of SHM can be used by the authority to improve the health of the population. In Russian history we have several examples where good intentions paved the way to undesirable effects. For example, if the Udmurtian authorities decide that alcohol abuse has the most detrimental effects on the Republic’s population – should they outlaw the production of alcohol? Or should they prohibit alcohol consumption in Udmurtia? Either decision may have untoward consequences.
For the moment, the Russian SHM system is considered to be mainly a passive information system, not a system for proactive response. To suggest to the politicians some alternatives for action within the sphere of public health, the system must also provide a possibility for impact assessment of such alternatives. Such assessment would be used to elaborate proper health care actions, to maximize positive effects, and to minimize negative effects.
As for now, it is especially important to reiterate that “the results of risk estimation shall not be used to adjust the payments to ecology funds, or by State Control institutions to impose sanctions” (Chief State Sanitary Physician of Russian Federation G. G. Onyshchenko and Chief State Inspector for Nature Protection of Russian Federation A. A. Solovianov (common document of 10.11.1997).
In general, the Russian system of medical informatics pertaining to environmental health is considered to be much more comprehensive than that of occupational health, on the level of primary data collection, as well as information analysis. Nevertheless, speaking of knowledge distribution level, the system is considered to be rather weak. The SHM system seems to be an isolated databank, its data are not likely to be often used even in other departments of The Healthcare Ministry, not saying about other Ministries or politicians.
Much more public attention should be driven to the SHM results to provide proper managerial decisions in sphere of public health, beneficial for the society.
6.1. The USA experience
In 1970 Congress passed the Occupational Safety and Health Act “to assure so far as possible every working man and woman in the Nation safe and healthful working conditions”. The National Institute for Occupational Safety and Health (NIOSH) was created to perform research concerning the causes of occupational injuries and illnesses and to make recommendations for the prevention of work-related disease and injury. To target national-wide research and prevention efforts, NIOSH uses a number of occupational health surveillance systems, including those developed on its own, as well as some external systems, e.g., the annual Survey of Occupational Injuries and Illnesses, conducted by the Bureau of Labor Statistics (BLS) since 1972. The information is collected using a scientifically selected probability sample from private U.S. industry establishments (about 165,000 establishments each year) [27]. The annual summary statistics can be found on the BLS website [28].
It should be mentioned that even the lists of recordable occupational diseases in the USA vary from state to state. There is no national registry of occupational illnesses or injuries, though now NIOSH is working with 36 states to develop state-based systems for surveillance of occupational disease and injury [5].
It is important to note that statistical data concerning occupational health in the USA are not always based on recordable cases alone, but are also based on special epidemiological studies are performed at targeted enterprises, performed in a manner so that the data can be extrapolated to the whole industry. This approach may allow for more reliable national-wide data than the data obtained from counting the recordable cases (which has the recognized limitations of underreporting and underregistering). There is a great temptation to introduce this approach in Russia immediately, but the first obstacle is lack of financing; the second obstacle is that the healthcare decision makers are not ready for such an approach. Still, as mentioned above, a positive indication for such an approach was given by healthcare authorities at the end of 2002 (the estimation of intrahospital infections for surveillance purposes). In light of the mentioned obstacles, some additional preparations are needed in the introduction of this practice concerning occupational injury and illness surveillance, for the ultimate goal of providing more reliable primary data on occupational morbidity.
It is important to mention, that in the USA a large number of different data sets on occupational and environmental health are fully available within the public domain, while in Russia, the public, journalists, and politicians do not have access to these data.
Environmental health data in the USA are collected mainly by the Environment Protection Agency; these data are also widely available, including access on the World Wide Web. There is an wide belief that a lack of public awareness of occupational and environmental health issues in Russia leads to an inability to suggest proper managerial and political decisions in these spheres.
The European countries have a long experience of collection, analysis and distribution of occupational and environmental health data.
The German Accident Insurance Act (from July 6, 1894), launched by the efforts of Otto von Bismarck, was the first of its kind in the world. The health insurance scheme, pension funds and so-called Berufsgenossenschaften (literally –occupational comradeships) were established in Germany by the end of XIX century.
Later, the system was adopted with some adjustment by the Scandinavian countries. By the end of XX century the experience of the Scandinavian countries – Sweden, Finland, and Denmark – in occupational and environmental health became recognized world-wide.
In Sweden, official statistics on occupational injuries have been available since 1906. Since 1918, the National Social Insurance Board was responsible for data collection on occupational health; since 1955, the data were officially published in the series Sveriges officiella statistic (Swedish Official Statistics). Currently, the data are collected by ISA (Work Injury Information System). The purpose of ISA is to provide supportive documentation for policies regarding a preventive work environment [28]. The statistics are generated from the data of a special work injury report form; this report is also filed with a public social insurance office. The ISA consists of a computerized registery and also an archive containing microfilms of work injury reports. The Swedish Work Environment Authority (SWEA) conducts special processing of primary data. The data with personal identifiers removed are available for individual researchers. The results can be found at SWEA website (www.av.se), as well as in the form of annual printed reports.
There was a special study performed in 1990s, which compared data from several survey studies of work-related health problems and registered work injuries. It was demonstrated that no more than about a half the cases that were presumed to be work-related illnesses were reported to ISA. It was also found that a certain percentage of so-called administrative dropouts existed (up to 21%),hen the health problems were reported to Social Insurance Office, but the data of the workers were not found in ISA later [29].
There is also Cancer registry, which collects data on cancer cases. As the occupation of a cancer patient is also registered, the Cancer registry can also be used for occupational health statistics, and has the ability to examine associations between cancer and certain occupations.
It is very important that the National Institute for Working Life (Arbetslivsinstitutet) is not concentrated only on working health issues, but covers a much wider spectrum of problems. One can speculate that it therefore has much better connections with political circles than most of the institutes in other countries (especially if compared with similar institutes in former socialist countries).
It can be seen that occupational health problems are well covered in the Swedish press currently, especially those dealing with issues of occupational stress, the health problems of office workers (e.g. due to indoor environmental quality, video display terminals, etc.). An interesting book named “Medicine in press and under press” was published by a collaborator of National Institute for Working Life in Malmö Dr. Bo Hagström [30]. The relationship between Swedish medicine and Swedish mass media are described in the book.
In general, the Swedish system of occupational data surveillance and analysis is probably one of the best in Europe, satisfying most of needs, and providing the decision makers with reliable, accurate data.
It should be emphasized that such a system was created because of decades of strong and productive cooperation between employers’ organizations and trade unions; such co-operation was also strongly endorsed and nurtured by governmental bodies.
Unfortunately, it seems that at present level of the political system in Russia, very few positive features of the Swedish system could be directly borrowed. Nevertheless, certain approaches might be replicated and, perhaps, the Russian trade unions could participate more actively in the planning stage of policy regarding the sphere of occupational health.
As an example of a former socialist country, Hungary still has its economy in transition, though few remains of socialist system can be seen now.
For example, the Hungarians have held onto the list of occupational diseases introduced in 1970s. Though there is a newer list of occupational diseases, which has been modified according to EU recommendations, workers with occupational diseases from the new list do not receive financial compensation yet.
There is a registry of occupational diseases in Hungary, led by the Institute of Occupational Health, as well as a system for biological monitoring of more than 30 hazardous chemicals. (In Russia, it is thought that it will take at least 10 years to develop a similar biological monitoring system. Sweden currently requires biological monitoring of only two chemicals – lead and cadmium). Annually, the Institute of Occupational Health publishes a special report on the state of occupational health in the country, based mainly on the registry data. Despite this timely information, there are still complaints that few necessary political decisions are based on the annual report data.
The Hungarian mass media has also remained uninterested in covering the problems of occupational and environmental health, unless there is some sensational case.
So, the Hungarian system seems to present the case where scientists possess all the necessary data, but have no opportunity to present them to society to focus more attention on the issue.
Historically Ukraine had strong connections with the same Soviet system of occupational and environmental health where the roots of the current Russian system began. Nevertheless, certain changes have taken place.
Being a smaller country than Russia, Ukraine did not need to implement the system requiring “regional centers for occupational medicine”, as did Russia in 1994. The Soviet system of the Research Institutes of Labor and Hygiene responsible for several neighboring regions has remained in the Ukraine. On one hand, it has prevented the creation of “regional centers” that lack the proper group of specialists in most fields of occupational medicine (e.g., occupational neurology, occupational surgery, occupational ophthalmology, etc.). On the other hand, presently, the Kharkhiv Institute of Labor Hygiene is responsible for e.g. Odessa region of Ukraine. This presents a problem, unfortunately, as illustrated by the 600 km distance between the occupational physicians and the workers who have to be under their care. Although there is no national occupational registry in Ukraine currently, there are registries in some regions. Work on implementation of a registry on national level has recently begun.
The caliber of work among certain Ukrainian occupational medicine physicians is much greater than the general level of occupational medicine in the country as a whole. This progression can be seen in the surveillance work concerning occupational and environmental exposure to ionizing radiation (the result of Chernobyl disaster) and the resultant health effects (Kiev Research Institute for Labor Medicine). Also, major advances can be seen in the collection and analysis of health data of computer users (Kharkiv Research Institute for Industrial Hygiene). In both Kiev and Kharkiv Institutes there has been surveillance of data occurring for more than 10 years.
During a recent visit to Kharkiv, there was a discussion devoted to introduction of the so-called “Health passport” in Ukraine. According the Healthcare Ministry Order, the “Health Passports” are individualized data banks kept on recordable CDs (CD-R) minidisks which catalogue patient information. These CD-R minidisks are to be kept by the citizens of Ukraine, and brought with them every time they seek medical care. The data from these visits are added to these disks after any new visit of the patient to the hospital/polyclinic.
Despite of approval of such a system, even by President Kuchma (as it was announced), it is difficult to understand how all the data (including X-ray images, ultrasound video etc.) will fit onto 180 MB minidisks. Each new cycle of adding information onto a CD-R disk requires at least 20-30 MB of additional service data.
With regards to mass media interest, unfortunately, occupational and environmental health is not a topic driving interest in Ukraine.
The following three items of reforms were suggested in the letter of the Nizhny Novgorod Research Institute for Hygiene and Occupational Pathology to the Health Care Committee of State Duma (The Lower Chamber of Parliament) of The Russian Federation. The letter described possible directions of reforms in occupational and environmental health, including the following proposals regarding medical informatics:
1. Development of a system to organize and carry out investigations to evaluate the most accurate, reliable, and valid occupational morbidity rate in Russia in order to guide managerial and political decisions aimed at the promotion of workers’ health.
Currently, the officially registered occupational morbidity in Russia is substantially less than that of industrially developed countries. The State Report “On Sanitary and Epidemiological Situation in the Russian Federation in 2000” pointed out that “incomplete documentation and surveillance of patients with occupational diseases were due to flawed labor safety legislation…, due to shortcomings in the organization and quality of preventive examinations of workers.” To reveal the true rates of occupational morbidity in Russia, special investigations should be organized and performed, using e.g., the American experience: carefully selecting representative enterprises in targeted industries and agriculture, and then carrying out investigations to better assess occupational morbidity at these enterprises. The results could then be extrapolated to the larger industrial sector.
The results of such a study would be used as a scientific base for managerial and political decisions aimed at worker health and safety prevention.
2. Development of computer software to create and conduct a national registry of patients with occupational diseases, and the implementation of this software in Federal and regional centers of occupational medicine in Russia.
Presently, there is no registry of patients with occupational diseases in Russia. Though the Social Insurance Fund conducts a data base of patients with occupational injury and illness who receive financial compensation, this database does not give a complete picture of occupational morbidity in Russia and its structure. Therefore, a surveillance system should be created in Russia to provide the systematic collection, analysis, interpretation, and dissemination of morbidity data which documents labor conditions, various occupational hazards, and possible occupational disability. This mechanism of a a continuing surveillance system, when implemented, will be able to be used to predict the state of occupational health in the country, as well as in separate regions.
3. The expansion of the scientific basis of modern telemedical technologies, enabling greater transfer of medical information through telecommunication channels which will then increase the availability of qualified medical service for inhabitants of the distant regions of Russia.
During last several years, telemedical technologies have been actively developed in Russia. The technologies have allowed qualified medical services to be available for certain populations in a few regions of Russia, where such services had not been available otherwise.
Nevertheless, certain problems with telecommunications exist: legal and some organizational questions remain unclear; there is no standardized scientific method or basis for telemedical consults. Establishing a standard methodology, and addressing legal concerns will help expand the use of modern telemedical technologies, hastening their implementation in the sphere of occupational and environmental health.
1. http://www.who.int/health_topics/medical_informatics/en (last checked February 7, 2003).
2. E. Coiera, Guide to medical informatics, the Internet and telemedicine. Chapman & Hall, 1997.
3. R. Gibson Parrish II, S. M. McDonnell. Sources of health-related information, in: Principles and practice of public health surveillance. Ed. by S. M. Teutsch, R. E. Churchill, Oxford University Press, 2000.
4. Leigh JP, Markowitz SB, Fahs M et al. Occupational injury and illness in the United States. Estimates of costs, morbidity, and mortality. Arch Intern Med 1997 Jul 28;157(14):1557-68.
5. Occupational health. Recognizing and Preventing Work-Related Disease and Injury. Ed. by B. S. Levy, D. H. Wegman. Lippincott, Williams & Wilkins, 1999.
6. I. Yurgens. Reform of social insurance system. Nezavisimaya gazeta, June 26, 2001(in Russian).
7. N. F. Izmerov, E. I. Denisov. Methodology of occupational risk assessment in labor medicine. In: Social and hygienic monitoring – practice and scientific basis. Moscow, 2000. P. 181-186 (in Russian).
8. http://www.health.gov/environment/DefinitionsofEnvHealth/ehdef2.htm (last checked February 7, 2003)
9. Occupational diseases: Handbook. Ed. by N. F. Izmerov. Moscow, 1996 (in Russian)
10. O. Vasiliev, S. Stepanov. Federal register of occupational diseases is needed. Meditsinsky vestnik, September 26, 2002 (in Russian).
11. On occupational morbidity in Russian Federation in 2001. Report of Federal Center for State Sanitary and Epidemiological Control. Moscow, 2002 (in Russian).
12. http://www.safework.ru/RISOT/tables/T1.htm (last checked February 7, 2003, in Russian)
13. Workers Health Chartbook, 2000. NIOSH, 2000.
14. http://www.dadp.dgu.ru/NS.htm (last checked February 7, 2003, in Russian)
15. E. Vlasova. Reform of insurance. Nezavisimaya gazeta, April 4, 2001(in Russian).
16. http://www.depart.drugreg.ru/doc/p_334_99.html (last checked February 7, 2003, in Russian)
17. V. M. Cherepov, D. I. Timokhin, O.V. Klepikov, V. V. Zhukova. Methodical approaches to building information systems for social and hygienic monitoring. In: Social and hygienic monitoring – practice and scientific basis. Moscow, 2000. P. 14-19 (in Russian).
18. http://www.gsen.ru/soft/expsoft/krista/sgm.html (last checked February 7, 2003, in Russian)
19. N.V. Matveev. Contemporary communication technologies in hygiene and occupational health. In: Social and hygienic monitoring – practice and scientific basis. Moscow, 2000. P. 80-84 (in Russian).
20. N. B. Harmancioglu, O. Fistioglu, S. D. Ozkul, M. N. Alpaslan. Decision making in environmental management. In: Environmental data management. Kluwer Academic Publishers, 1998.
21. http://www.sra.org/ gloss3.htm#R (last checked February 7, 2003)
22. S. A. Melyuk, N. L. Karpov, N. A. Solonenko. Software and hardware for social and hygienic monitoring. In: Social and hygienic monitoring – practice and scientific basis. Moscow, 2000. P. 90-95. (in Russian).
23. N. A. Zabrodin, N. A. Kirianov, R. A. Kharten. Ranking the risk factors for population health. . In: Social and hygienic monitoring – practice and scientific basis. Moscow, 2000. P. 230-233. (in Russian).
24. V. F. Spirin, M. A. Mironenko, A. D. Doblo. Hygienic priorities social and hygienic monitoring in rural area. . In: Social and hygienic monitoring – practice and scientific basis. Moscow, 2000. P. 137-141. (in Russian).
25. Yu. P. Tikhomirov, M. P. Gracheva, I. V. Fedotova et al. On methodology of estimation of technogenic risk for female reproductive health. In: Ecological and environmental problems of population health preservation. Nizhny Novgorod, 1999 (in Russian).
26. http://www.fcgsen.ru (last checked February 7, 2003, in Russian)
27. A NIOSH look at data from the Bureau of Labor Statistics. NIOSH, 2000.
28. http://www.bls.gov/iif/home.htm#tables (last checked March 17, 2003)
29. ISA- The Swedish Information System for Occupational Accidents and Work-Related Diseases. SWEA Rapport 2000:16.
30. The information system for Occupational Injuries and the Work-related Health Problem Survey. Statistics Sweden 2002:2.
31. Bo Hagström. Svensk sjukvård i och under press. Studentlitteratur, Lund, 2002 (in Swedish).
Occupational diseases have been more precisely studied and categorized, than environmental diseases; therefore it is easier to estimate the loss due to occupational diseases. For example, the investigation performed in the USA [4] demonstrated that approximately 862,200 occupationally related illnesses were estimated to occur annually in the civilian American workforce. The total direct ($65 billion) plus indirect ($106 billion) costs were estimated to be $171 billion. Injuries cost $145 billion and illnesses $26 billion. These estimates did not take into account costs associated with pain and suffering, as well as costs associated with in-home care provided by family members. Overall, because of the inadequacy of surveillance of disease the numbers of occupational and illnesses are likely to be underestimated.
Comparatively, the economical burden of AIDS was estimated at $33 billion, $57 billion for Alzheimer’s disease, $164 billion for circulatory diseases, and $171 for cancer.
Unfortunately, no official estimates are currently available for Russia. The rough estimates are derived from the above-mentioned U.S. figures, and are based on the two following assumptions:
1) the economic burden due to occupational illnesses is directly related with national GDP level (reflecting the overall production level of the national economy).
2) the economic burden is associated with the registered numbers of occupational patients per annum.
The ratio of the US GDP/Russia GDP was approximately 20 (for 1994). If we assume that the occupational morbidity in Russia and the USA is roughly similar, Russian economic loss due to occupational illnesses might total $8 billion ($3 billion direct and $5 billion indirect). Still, there is a great difference between the figures of occupational morbidity in the countries: US Bureau of Labor Statistics reported 429,800 new cases of occupational diseases in private industry in 1999 [5]. The Russian Federal Center of State Committee for Sanitary and Epidemiological Control reported 283,851 cases of occupational illnesses in Russian Federation during last 30 years (1972-2001) [11]. If we assume this Russian figure to be correct, we have to assume that the economic burden due to occupational illnesses in Russia is substantially less (45 times) than the calculated estimation of $8 billions – about $170 million. Given that the latest modest figures are reliable, and these figures reflect the actual societal burden correctly, we might agree that little attention is paid by society to the problem of OEH. But only the expenditures of the Russian Fund of Social Insurance in 2000 were 12 billion RUR [6] – approximately $400 mln., or significantly higher than our “optimistic” estimation. The most pessimistic estimate was made by the chief Russian specialist in occupational health, academician N. F. Izmerov, who reported it to be “10-20% of Russian GDP” [7].
Nevertheless, a major question is whether Russian figures of occupational morbidity are reliable. This question will be discussed in more detail below.
The problem of economic burden estimation due to environmental health disorders is even more complicated than the assessment of occupational illness burden, mainly due to the fact that the definition of environmental illness (health disorder) is unclear, or at least not as fully developed as the definition of occupational disease.
WHO stated (draft definition developed at a WHO consultation in Sofia, Bulgaria, 1993): “Environmental health comprises of those aspects of human health, including quality of life, that are determined by physical, chemical, biological, social, and psychosocial factors in the environment. It also refers to the theory and practice of assessing, correcting, controlling, and preventing those factors in the environment that can potentially affect adversely the health of present and future generations”. It should be mentioned that there are at least 27 other definitions of environmental health [8].
It is obvious that a person may inhabit a series of different environments in the course of his life or even in the course of the day. Ambient environments vary by geography and may vary markedly even within a single city.
A broad spectrum of agents has been associated with chronic health effects in the population. For example:
- Ambient air pollutants (ozone, particulate matter, toxic chemicals, etc.)
- Indoor air pollutants (formaldehyde, carbon monoxide, tobacco smoke, etc.)
- Pesticide resides in food (some of them are suspected carcinogens)
- Disinfection byproducts in drinking water.
It is important to note that the relationship between the environment and health status is modified by many factors (e.g., age, sex, genetic makeup, state of health, dietary habits, etc.), so in general, an individual’s health response to environmental factors can be very different. So, a strict legal definition of the term “environmental disease” remains elusive. This dilemma explains the hardship in establishing the connection between environmental factors influence and resulting health disorders. Often the direct relationship for a single individual cannot be found, and in such cases, the relationship may be revealed only using statistical methods.
Currently, we live in an age of environmental alertness. The social (and political) importance of environmental health cannot be overestimated. Environmental health impacts a wide strata of the population, or rather, the population at large (i.e., if we discuss the problem of ambient air pollution). At the same time, occupational health is actually only a small part of environmental health, as the occupational environment is just a small part of the environment as a whole.
The issues regarding responsibility for health disorders due to environmental factors (especially, anthropogenic environment pollution) can be seen as very acute; especially now, when attention of society has been largely focused on environmental issues. There is a fragile balance that exists between the interests of industry and the interests of the population exposed to the industrial pollutants. The balance of the interests should be established mainly by political processes.
There are two main types of primary data in occupational health – the data regarding work conditions of an individual worker and the data which focuses on his/her health status. In Russia, the data on work conditions (the hygienic characteristics of workplace) are collected by local centers of sanitary and epidemiological control. The person responsible is usually an industrial hygienist, who may either use the available data on working conditions at the specific enterprise, or conduct a workplace evaluation (e.g., measure ambient air in a workplace for concentrations of chemical substances). The data on working conditions are presented to the occupational physician, to whom the worker is referred. The occupational physician, usually in a Regional/Republican Center of Occupational Pathology, compares clinical findings and medical records of the patient with the industrial hygiene data. Then, a determination is made by a commission of the Center of Occupational Pathology (according to the proper normative documents issued by the Healthcare Ministry of Russian Federation) whether a person has or does not have an occupational disease.
Obligatory registration of patients with occupational diseases in Russia was introduced as early as in 1924 [9]. Until 1986, the reports of registered occupational diseases were submitted quarterly by local sanitary and epidemiological stations (later renamed “centers of sanitary and epidemiological control”). Since 1986, individual registration of new cases of occupational diseases began, not just number of cases for each enterprise or territory. The system of registration was automated, which enabled easier analysis of the data. Some regions of Russia introduced more complex computerized systems of registration and analysis of occupational diseases, which were able to perform deeper statistical analysis [9].
According to the Order of Healthcare Ministry of Russian Federation #130 (of 23.06.1994), the system of Centers for Occupational Pathology was created. Previously (during the Soviet years), a system of several Research Institutes of Hygiene had to provide occupational health services for all the Russian workers, but the Institutes were too few and too distant from many of industrial centers to cover the needs in post-Soviet Russia.
Newly created Centers for Occupational Pathology were tasked with creating data banks on occupational morbidity, mortality, and disability. Nevertheless, at some territories the new Centers were not created (e.g., Vladimir region), and some regions’ “Centers” consisted of no more than 2-3 physicians, and were not real centers in the full sense of the word (e.g., there was a single occupational physician working part-time in Mari El Republic with population of 750,000).
Virtually, now there are several parallel systems of registration of occupational diseases functioning in Russia:
1) within the system of Centers for Occupational Pathology (led at the federal level by the Research Institute of Labor Medicine of Russian Academy of Medical Sciences) – the origin of primary data;
2) within the system of the Centers for State Sanitary and Epidemiological Control (led by the Federal Center);
3) within the Ministry of Labor and Social Security;
4) in the Fund of Social Insurance against Occupational Injures and Diseases
The need for the integrated Registry of Occupational Diseases was discussed in Russia for several years, but the creation of the Registry is still in the process.
Beginning in 2001, the first approaches toward the creation of the Registry were published. According to the published data [11], The State Registry of Occupational Diseases in the Russian Federation should be “a system for active dynamic surveillance over the patients with registered occupational disorders in order to:
1) preserve the worker’s health and capacity to work ;
2) provide full compensation of health impairment or disability;
3) minimize the causes for occupational disorders;
4) develop and implement economically feasible mechanisms for improvement of working conditions;
5) develop and implement the state policy toward preservation of workers’ health”.
Unfortunately, until now, the occupational statistics are limited only to the registration of new cases of occupational diseases. Summary statistics are not available yet, which prevents not only estimation of total national burden due to occupational disorders, but also prevents follow-up of occupational cases (if it results in disability or not, etc.). Currently, the newly created Fund of Social Insurance against Occupational Injuries and Diseases has surveillance data only on a portion of occupational patients, those who have been compensated. Still, this system only reaches a part of all occupational patients. The workers who just leave their workplaces due to occupational diseases, but do not receive any material compensation, miss the records of Fund of Social Insurance.
In general, several problems are well-known, preventing adequate surveillance of occupational cases in most countries:
- employers are not interested reporting of occupational cases (even if compensation to workers with occupational diseases is not paid directly by them, higher figures of occupational morbidity at the individual enterprise may result in higher employers’ payments to the social security institutions);
- employees are also not always interested in reporting of work related illness or injury (official registration of disease might mean leaving a rather lucrative job and may also create a hardship in searching for a new job).
In Russia, some additional negative factors may also be present:
- There was a tradition of unreliable statistics during Soviet times. (Until Perestroika, the official figures of occupational morbidity had to be decreased year by year, despite whatever reality existed, to prove the “superiority” of the socialist system. A demonstrative example can be illustrated with a situation at a chemical plant in Nizhny Novgorod region, where all cases of contact eczema were registered as “viral respiratory disorders” – so that the workers could leave work connected with handling allergens for several days without “worsening” local occupational statistics.
- Currently, a “black-market economy” forms a significant part of the Russian economy (according to some estimates, up to 40%), so a portion of workers are considered to be unemployed, but actually, they are employed at some black-market enterprise, where they might be handling some hazardous factors. Surely, such workers would never be eligible for any compensation in case of their disease or injury, and no occupational health statistics is available for this significantly large group of workers in Russia.
- A rather low level of monetary compensation for cases of occupational disorders may keep workers from applying although, on the other hand, excessive compensation might inflate the actual number of occupationally diseased workers).
- The number of physicians allowed to diagnose occupational disease is insufficient (in Russia, only occupational physicians working in Centers for Occupational Pathology are allowed to make diagnosis of occupational disease, and the number of such physicians is less than 1,000, while in the US, there are at least 2,400 physicians certified in occupational medicine [5]).
- Few workers possess the knowledge to wade through the bureaucracy of the occupational insurance and compensation system in Russia, often they are not aware of their rights, and sometimes they might be mislead by their administration (very little attention is paid to occupational topics by mass media, including newspapers, television, and Internet sites).
The latest available figures of occupational morbidity in Russia seem to be too low to be correct – 2.24 per 10,000 employees (official data for 2001 [11, 12]).
At the same time in the USA, this figure was 49.8 illnesses per 10,000 full-time workers [13], a 22-fold increase compared to Russia. This increase cannot be explained by better working conditions in Russia – officially, up to 25% of all working places in Russia do not comply with industrial hygiene requirements [12]. The differences might be slightly less dramatic, when one takes into account that the US index is calculated per 10,000 full-time workers, while Russian index is calculated per 10,000 total workers, and the number of part-time workers at current economic conditions of Russia is substantial.
A scientific assessment should be performed in Russia to capture a more reliable and accurate occupational morbidity, which according to rough estimates, should be considered at least at the level of other industrially developed countries (e.g., the USA), but may even exceed the figures reported in Western countries. As occupational mortality in the USA is about 4 times less than the index found in Russia, we should expect a similar ratio between occupational morbidity – or, approximately, a 90-fold underreporting of occupational diseases in Russia.
It is interesting to compare the registration of occupational morbidity with the registration of intrahospital infections in Russia. There has been usual controversy regarding the official statistics of intrahospital infections as well. Recently The Chief Sanitary Physician of Russian Federation, G. G. Onishchenko, in his Decree #37 (of 06.11.2002), in reference to the data found in the investigation of the registered number of intrahospital infections), stated that the official number was approximately 50 times less than the real number. His decree was an honest attempt to try to correct what he saw was a blatant underestimation of the scope of disease, although it disputed the officially sanctioned statistical data.
The analysis of occupational health information is mainly a comparison of working condition data and workers’ health data. Being compared, the data provides healthcare professionals with information on occupational risks.
The following definition of the term “occupational risk” is given by Federal Law “On obligatory social insurance against occupational injuries and diseases”: “The occupational risk is the probability of a health disorder (loss) or death, connected with carrying out the duties according to labor contract (or in other cases, stated by law)”.
Speaking of occupational risks evaluation, it should be mentioned that the first computerized systems for this were created in 1970s. The Latvian system KASMON was introduced at the USSR level in 1980s. The “occupational health unit” was available for KASMON system, written in BASIC. Now more up-to date computerized systems are used in Russian occupational health. At the moment, the Research Institute of Labor Medicine (in Moscow) prepares “The handbook on occupational risk assessment”. In this handbook the issues of occupational risk due to noise, vibration, dust and some other hazardous factors will be covered [9].
The evaluation of occupational risks is very popular now in Russian medical science. During 2002, 18 Russian articles covering the topic of occupational risk were quoted by MedLine. The occupationally-related risks of coronary heart disease, arterial hypertension, carcinogenic effects, occupational bronchopulmonary diseases, reproductive disorders, etc. were included.
Though the methodology of occupational risk estimation is well known, there is an opinion that the risk estimation must not be correct if it is based on unreliable occupational morbidity data [15]. Perhaps, this explains a rather skeptical attitude toward the occupational risk estimation methodology. It is clear that if morbidity figures are still unreal, risk estimation based on the figures is also far from being correct, so the practical measures suggested according to the estimations will always be questionable for society.
Meanwhile, currently the occupational risk data are not supposed to be used by Social Insurance Fund to calculate the employers’ dues, only the number of registered occupational diseases is used compared to the number of them during previous year [14].
Unlike in most industrially developed countries, the topic of occupational health is not one that receives much public attention in Russia. This lack of public and media attention can be seen by comparing the number of media stories run on occupational health in leading Russian and American newspapers.
In “Rossiyskaya Gazeta” (“The Russian Newspaper”, one of the most influential and widely circulated newspapers of Russia), from 2001 to March 2003, only 6 articles mentioning the key terms “occupational diseases” were found (no full analogue of the English language term “occupational health” is available in Russian language). At the same time, on the website of “USA Today” 312 entries searched by the terms “occupational health” were found for the same period. In several instances, the articles addressing occupational health topics appeared on the front page of several American newspapers as the “lead stories” (e.g., the article “Court to decide scope of disabilities act” appeared on front page of “USA Today” on 04.17.2001). Such a prominent place rarely, if ever, has occurred regarding an article on occupational health in the Russian press.
It can also be demonstrated that virtually no information on occupation health and safety is available on the websites of the Russian Trade Unions or any of the political parties (including even the left-wing parties).
In summarizing the general impression of today’s state of health informatics within the occupational health system of Russia, we must explicitly state that the system is unsuitable for the current needs of Russian society – it is generally based on old-style Soviet principles, and strongly needs to be up-dated. There are some positive “seeds” in the system, such as the risk assessment methodology, that must be kept; but the system of primary data collection should be restructured. Other measures should also be taken to draw the attention of the Russian society (in particular, the trade unions, journalists, and politicians) to the opportunities that occupational health offers in promoting health and quality of life by preventing and controlling workplace disease, injury, and disability.
In the 1990s, the system of social and hygienic monitoring (SHM) was launched in Russia.
The legal basis for the SHM system originated from the “Statement on Social and Hygienic Monitoring”, which was approved by RF government on June 1, 2000. “The Statement” described SHM as “the state system of surveillance, analysis, estimation and prognosis of the state of population health and human environment”. The same statement established the Federal Information Fund of SHM data as “the repository for data on the state of population health and human environment, which includes information acquired through long-term surveillance, as well as legal documents and reference materials on the analysis, prognosis and relationship between environmental factors and human health.”
The primary data are collected in their entirety: population health indices, social and economical indices, ambient air pollution, drinking water quality. According to Order # 334 of the Healthcare Ministry of Russian Federation (of 27.08.1999), there are two levels of data represented:
- from the local level to the regional level;
- from the regional level to the Federal level.
There is a comprehensive list of the health, social and hygienic indices to be used [16]. The indices provide mainly basic statistical information, whose standard methodologies have been utilized for decades (e.g., mortality indices). There are also data on environmental pollutants from the most widely used chemicals. Because most of such indices are based on standard measurable outcomes (e.g., specific levels of chemicals or number of deaths from specific causes) they may be more accurate and reliable than e.g. occupational morbidity data.
The SHM system inherited the ideas of some previous systems for health effects surveillance. For example, by the end of 1990s the system of birth defects registration was created in Russia (based on several normative documents, including The Order of Healthcare Ministry #268 of 10.09.1998). Unfortunately, initially the data of birth defects were collected in the regions of Russia without any connection with pollution data. Currently the comparisons between environmental pollution and birth defects rate can be performed.
Russian investigators V. M. Cherepov, D. I. Timokhin, O.V. Klepikov, V. V. Zhukova (2000) have emphasized that SHM data should be detailed enough to allow their use in making effective managerial decisions [17]. However, according to the same authors, there are some specific features which might limit the possible use of the SHM system:
- the character of the data and their variability;
- the limitations of the algorithms used for making managerial decisions;
- the technical limitations;
- a time lag between the collection of the data and their analysis and publication;
- a time lag before any intervention evaluation can be performed;
- lack of cost-effectiveness of the informational systems;
- inherent complexities of social and political interpretation of the data.
It should also be mentioned that there is controversy involving the need for the timely flow of information versus the accuracy and reliability that comes with this faster transfer of information. Two approaches have been mentioned – first, whether to limit the raw data at the input level (to prevent the “flood” of data at the higher levels), or second, to allow the passage of the raw data directly to the higher level, which would then provide some data verification and analysis. The first approach would be preferred if the primary level of data collection were made fully reliable, and then at least, partial analysis of the data could be performed at this level.
Usually, the supposition is that the higher levels of organizations or government (regional, Federal) are better equipped and have more qualified personnel to a more thorough analysis of raw data.
Specific software was designed to provide data flow within the SHM system. Perhaps one of the best is the automated system “Social and hygienic monitoring”, developed by “Krista”, a software company of Rybinsk, Yaroslavl region [18]. This is a distributed database, which is able to provide SHM data flow within the whole region (from local districts to regional offices, and finally, to the Federal level), and it fulfills the requirements of the Healthcare Ministry with regards to SHM. It is adaptable to the needs of specific users, and certain features can be added upon users’ request.
Russian medical scientists and authors from other countries have suggested that it would be advantageous if certain environmental data (e.g., air and water pollutants) were collected by automated quantitative sampling devices, so that the data could not be tampered with or falsified by personnel [19, 20].
According to “Statement on Social and Hygienic Monitoring”, the aims of SHM system in Russian Federation are the following:
- to document and assess risk factors able to cause harmful effects on human health;
- to identify, evaluate, assess and predict the state of human health and environment;
- to define urgent and long-term measures for prevention of harmful environmental effects on human health;
- to formulate recommendations on controlling and reduction of exposures, illness, and injury regarding human health and environment
- to disseminate information to state and local authorities, other institutions, and the citizens on the SHM results.
The concept of SHM is based on the principles of environmental risk assessment which were introduced by the Chief State Sanitary Physician of Russian Federation G. G. Onyshchenko and Chief State Inspector for Nature Protection of Russian Federation, A. A. Solovianov (common document of 10.11.1997). It was stated that at the beginning of the work on environmental risk assessment in Russia, the U.S. EPA experience would be widely used, after adjusting for Russian conditions. The project was sponsored by some international organizations, e.g., US Agency for International Development, International Bank for Reconstruction and Development.
The term “risk” as defined was very close to the definition given in the U.S. EPA glossary: “The potential for realization of unwanted, adverse consequences to human life, health, property, or the environment; estimation of risk is usually based on the expected value of the conditional probability of the event occurring times the consequence of the event given that it has occurred” [21].
Using the SHM system information on a regional level, many regions of Russia were able to calculate environmental risks, or were able to compare the environmental risks with other health risks. One of the first regions able to perform such analysis was the Yaroslavl region, where the above mentioned SHM software was introduced [22]. Some interesting data were obtained in Udmurtian Republic [23] on risk factors associated with adverse health effects among the Udmurtian population. For example, it was found that alcohol abuse increased the risk of overall health disorders 3.1 times, smoking increased the risk 2.9 times, environmental pollution increased the risk 1.8 times. In Saratov region, nine main risk factors were identified, associated with the occurrence of overall health disorders in the population [24]:
1) Pesticide-containing food products (18.8%);
2) Air pollution at work (16.4%);
3) Nitrate containing food products (12.8%);
4) Marriage status (11.2%);
5) Air pollution at home (10.7%);
6) Elevated noise levels at home (8.2%);
7) Water pollution (7.6%);
8) Elevated noise levels at working place (5.9%);
9) Poor living conditions (4.7%).
Investigators of the Nizhny Novgorod Research Institute for Hygiene and Occupational Pathology reported on the health status of approximately 1000 newborn infants in one of the main centers of Russian chemical industry, Dzerzhinsk [25]. Children of the mothers handling potentially teratogenic chemicals at work were found to have slightly better performance and health indices than children born from mothers who had never worked in the chemical industry. Although the results seemed unexpected, the differences in income rates offered some explanation. According to these additional data, mothers working in chemical industry had much better salaries than those who never worked with chemicals (teachers, librarians etc.). This example supports the assertion that the data for SHM should be as detailed as possible, and should be analyzed in their entirety, without missing social indices.
Missing the comprehensive nature of the data may result in neglecting some important aspects of human health.
Some examples of the use of existing data based on the SHM system were given above. We suppose that SHM data might be used to rank previously identified risk factors, rather then finding new ones. For example, if we look at the list of potential risk factors provided for Saratov region [24], it can be agreed that all the factors listed were considered to be harmful decades ago. Still, the importance and impact of social factors (e.g., salary rate) upon health outcomes has recently been introduced into the social consciousness in Russia. After many decades of declared “social equality”, it has taken some time for the importance of social factors’ impact on public health to be officially acknowledged.
SHM system is rarely discussed in public; now it seems to remain just a working system inside The Healthcare Ministry of Russian Federation.
Though “The Statement on Social and Hygienic Monitoring” described that one of the aims of the SHM system to be “to inform state and local authorities, other institutions and the citizens on the SHM results”, little information on these results is available, excepting several proceedings of the scientific conferences, published as no more than 1500 copies.
The mass media seldom pays attention to so “dull” a topic; it usually focuses only on events such as large-scale environmental disasters. On the Internet, the most interesting information could be found at the website of the Federal Center of State Sanitary and Epidemiology Control [26], but SHM data are restricted from the public viewing by password protection and is available only to certain healthcare authorities.
The ability of managers to use the SHM system to make improvements in the quality of health care will be the single best criterion in evaluating its effectiveness [17]. Nevertheless, if the ability to use the system is delayed (and part of its utility will necessarily be delayed for decades – e.g., in case of tracing the carcinogenic activity of some identified pollutants) – the efficacy of the system as a whole will remain questionable.
Unfortunately, neither “The Statement on Social and Hygienic Monitoring” nor other government documents delineate how the results of SHM can be used by the authority to improve the health of the population. In Russian history we have several examples where good intentions paved the way to undesirable effects. For example, if the Udmurtian authorities decide that alcohol abuse has the most detrimental effects on the Republic’s population – should they outlaw the production of alcohol? Or should they prohibit alcohol consumption in Udmurtia? Either decision may have untoward consequences.
For the moment, the Russian SHM system is considered to be mainly a passive information system, not a system for proactive response. To suggest to the politicians some alternatives for action within the sphere of public health, the system must also provide a possibility for impact assessment of such alternatives. Such assessment would be used to elaborate proper health care actions, to maximize positive effects, and to minimize negative effects.
As for now, it is especially important to reiterate that “the results of risk estimation shall not be used to adjust the payments to ecology funds, or by State Control institutions to impose sanctions” (Chief State Sanitary Physician of Russian Federation G. G. Onyshchenko and Chief State Inspector for Nature Protection of Russian Federation A. A. Solovianov (common document of 10.11.1997).
In general, the Russian system of medical informatics pertaining to environmental health is considered to be much more comprehensive than that of occupational health, on the level of primary data collection, as well as information analysis. Nevertheless, speaking of knowledge distribution level, the system is considered to be rather weak. The SHM system seems to be an isolated databank, its data are not likely to be often used even in other departments of The Healthcare Ministry, not saying about other Ministries or politicians.
Much more public attention should be driven to the SHM results to provide proper managerial decisions in sphere of public health, beneficial for the society.
6. Possible use of foreign experience in reform of information flow within Russian system of occupational and environmental health
6.1. The USA experience
In 1970 Congress passed the Occupational Safety and Health Act “to assure so far as possible every working man and woman in the Nation safe and healthful working conditions”. The National Institute for Occupational Safety and Health (NIOSH) was created to perform research concerning the causes of occupational injuries and illnesses and to make recommendations for the prevention of work-related disease and injury. To target national-wide research and prevention efforts, NIOSH uses a number of occupational health surveillance systems, including those developed on its own, as well as some external systems, e.g., the annual Survey of Occupational Injuries and Illnesses, conducted by the Bureau of Labor Statistics (BLS) since 1972. The information is collected using a scientifically selected probability sample from private U.S. industry establishments (about 165,000 establishments each year) [27]. The annual summary statistics can be found on the BLS website [28].
It should be mentioned that even the lists of recordable occupational diseases in the USA vary from state to state. There is no national registry of occupational illnesses or injuries, though now NIOSH is working with 36 states to develop state-based systems for surveillance of occupational disease and injury [5].
It is important to note that statistical data concerning occupational health in the USA are not always based on recordable cases alone, but are also based on special epidemiological studies are performed at targeted enterprises, performed in a manner so that the data can be extrapolated to the whole industry. This approach may allow for more reliable national-wide data than the data obtained from counting the recordable cases (which has the recognized limitations of underreporting and underregistering). There is a great temptation to introduce this approach in Russia immediately, but the first obstacle is lack of financing; the second obstacle is that the healthcare decision makers are not ready for such an approach. Still, as mentioned above, a positive indication for such an approach was given by healthcare authorities at the end of 2002 (the estimation of intrahospital infections for surveillance purposes). In light of the mentioned obstacles, some additional preparations are needed in the introduction of this practice concerning occupational injury and illness surveillance, for the ultimate goal of providing more reliable primary data on occupational morbidity.
It is important to mention, that in the USA a large number of different data sets on occupational and environmental health are fully available within the public domain, while in Russia, the public, journalists, and politicians do not have access to these data.
Environmental health data in the USA are collected mainly by the Environment Protection Agency; these data are also widely available, including access on the World Wide Web. There is an wide belief that a lack of public awareness of occupational and environmental health issues in Russia leads to an inability to suggest proper managerial and political decisions in these spheres.
The European countries have a long experience of collection, analysis and distribution of occupational and environmental health data.
The German Accident Insurance Act (from July 6, 1894), launched by the efforts of Otto von Bismarck, was the first of its kind in the world. The health insurance scheme, pension funds and so-called Berufsgenossenschaften (literally –occupational comradeships) were established in Germany by the end of XIX century.
Later, the system was adopted with some adjustment by the Scandinavian countries. By the end of XX century the experience of the Scandinavian countries – Sweden, Finland, and Denmark – in occupational and environmental health became recognized world-wide.
In Sweden, official statistics on occupational injuries have been available since 1906. Since 1918, the National Social Insurance Board was responsible for data collection on occupational health; since 1955, the data were officially published in the series Sveriges officiella statistic (Swedish Official Statistics). Currently, the data are collected by ISA (Work Injury Information System). The purpose of ISA is to provide supportive documentation for policies regarding a preventive work environment [28]. The statistics are generated from the data of a special work injury report form; this report is also filed with a public social insurance office. The ISA consists of a computerized registery and also an archive containing microfilms of work injury reports. The Swedish Work Environment Authority (SWEA) conducts special processing of primary data. The data with personal identifiers removed are available for individual researchers. The results can be found at SWEA website (www.av.se), as well as in the form of annual printed reports.
There was a special study performed in 1990s, which compared data from several survey studies of work-related health problems and registered work injuries. It was demonstrated that no more than about a half the cases that were presumed to be work-related illnesses were reported to ISA. It was also found that a certain percentage of so-called administrative dropouts existed (up to 21%),hen the health problems were reported to Social Insurance Office, but the data of the workers were not found in ISA later [29].
There is also Cancer registry, which collects data on cancer cases. As the occupation of a cancer patient is also registered, the Cancer registry can also be used for occupational health statistics, and has the ability to examine associations between cancer and certain occupations.
It is very important that the National Institute for Working Life (Arbetslivsinstitutet) is not concentrated only on working health issues, but covers a much wider spectrum of problems. One can speculate that it therefore has much better connections with political circles than most of the institutes in other countries (especially if compared with similar institutes in former socialist countries).
It can be seen that occupational health problems are well covered in the Swedish press currently, especially those dealing with issues of occupational stress, the health problems of office workers (e.g. due to indoor environmental quality, video display terminals, etc.). An interesting book named “Medicine in press and under press” was published by a collaborator of National Institute for Working Life in Malmö Dr. Bo Hagström [30]. The relationship between Swedish medicine and Swedish mass media are described in the book.
In general, the Swedish system of occupational data surveillance and analysis is probably one of the best in Europe, satisfying most of needs, and providing the decision makers with reliable, accurate data.
It should be emphasized that such a system was created because of decades of strong and productive cooperation between employers’ organizations and trade unions; such co-operation was also strongly endorsed and nurtured by governmental bodies.
Unfortunately, it seems that at present level of the political system in Russia, very few positive features of the Swedish system could be directly borrowed. Nevertheless, certain approaches might be replicated and, perhaps, the Russian trade unions could participate more actively in the planning stage of policy regarding the sphere of occupational health.
As an example of a former socialist country, Hungary still has its economy in transition, though few remains of socialist system can be seen now.
For example, the Hungarians have held onto the list of occupational diseases introduced in 1970s. Though there is a newer list of occupational diseases, which has been modified according to EU recommendations, workers with occupational diseases from the new list do not receive financial compensation yet.
There is a registry of occupational diseases in Hungary, led by the Institute of Occupational Health, as well as a system for biological monitoring of more than 30 hazardous chemicals. (In Russia, it is thought that it will take at least 10 years to develop a similar biological monitoring system. Sweden currently requires biological monitoring of only two chemicals – lead and cadmium). Annually, the Institute of Occupational Health publishes a special report on the state of occupational health in the country, based mainly on the registry data. Despite this timely information, there are still complaints that few necessary political decisions are based on the annual report data.
The Hungarian mass media has also remained uninterested in covering the problems of occupational and environmental health, unless there is some sensational case.
So, the Hungarian system seems to present the case where scientists possess all the necessary data, but have no opportunity to present them to society to focus more attention on the issue.
Historically Ukraine had strong connections with the same Soviet system of occupational and environmental health where the roots of the current Russian system began. Nevertheless, certain changes have taken place.
Being a smaller country than Russia, Ukraine did not need to implement the system requiring “regional centers for occupational medicine”, as did Russia in 1994. The Soviet system of the Research Institutes of Labor and Hygiene responsible for several neighboring regions has remained in the Ukraine. On one hand, it has prevented the creation of “regional centers” that lack the proper group of specialists in most fields of occupational medicine (e.g., occupational neurology, occupational surgery, occupational ophthalmology, etc.). On the other hand, presently, the Kharkhiv Institute of Labor Hygiene is responsible for e.g. Odessa region of Ukraine. This presents a problem, unfortunately, as illustrated by the 600 km distance between the occupational physicians and the workers who have to be under their care. Although there is no national occupational registry in Ukraine currently, there are registries in some regions. Work on implementation of a registry on national level has recently begun.
The caliber of work among certain Ukrainian occupational medicine physicians is much greater than the general level of occupational medicine in the country as a whole. This progression can be seen in the surveillance work concerning occupational and environmental exposure to ionizing radiation (the result of Chernobyl disaster) and the resultant health effects (Kiev Research Institute for Labor Medicine). Also, major advances can be seen in the collection and analysis of health data of computer users (Kharkiv Research Institute for Industrial Hygiene). In both Kiev and Kharkiv Institutes there has been surveillance of data occurring for more than 10 years.
During a recent visit to Kharkiv, there was a discussion devoted to introduction of the so-called “Health passport” in Ukraine. According the Healthcare Ministry Order, the “Health Passports” are individualized data banks kept on recordable CDs (CD-R) minidisks which catalogue patient information. These CD-R minidisks are to be kept by the citizens of Ukraine, and brought with them every time they seek medical care. The data from these visits are added to these disks after any new visit of the patient to the hospital/polyclinic.
Despite of approval of such a system, even by President Kuchma (as it was announced), it is difficult to understand how all the data (including X-ray images, ultrasound video etc.) will fit onto 180 MB minidisks. Each new cycle of adding information onto a CD-R disk requires at least 20-30 MB of additional service data.
With regards to mass media interest, unfortunately, occupational and environmental health is not a topic driving interest in Ukraine.
7. The main possibilities for reforming information data flow in occupational and environmental health
The following three items of reforms were suggested in the letter of the Nizhny Novgorod Research Institute for Hygiene and Occupational Pathology to the Health Care Committee of State Duma (The Lower Chamber of Parliament) of The Russian Federation. The letter described possible directions of reforms in occupational and environmental health, including the following proposals regarding medical informatics:
1. Development of a system to organize and carry out investigations to evaluate the most accurate, reliable, and valid occupational morbidity rate in Russia in order to guide managerial and political decisions aimed at the promotion of workers’ health.
Currently, the officially registered occupational morbidity in Russia is substantially less than that of industrially developed countries. The State Report “On Sanitary and Epidemiological Situation in the Russian Federation in 2000” pointed out that “incomplete documentation and surveillance of patients with occupational diseases were due to flawed labor safety legislation…, due to shortcomings in the organization and quality of preventive examinations of workers.” To reveal the true rates of occupational morbidity in Russia, special investigations should be organized and performed, using e.g., the American experience: carefully selecting representative enterprises in targeted industries and agriculture, and then carrying out investigations to better assess occupational morbidity at these enterprises. The results could then be extrapolated to the larger industrial sector.
The results of such a study would be used as a scientific base for managerial and political decisions aimed at worker health and safety prevention.
2. Development of computer software to create and conduct a national registry of patients with occupational diseases, and the implementation of this software in Federal and regional centers of occupational medicine in Russia.
Presently, there is no registry of patients with occupational diseases in Russia. Though the Social Insurance Fund conducts a data base of patients with occupational injury and illness who receive financial compensation, this database does not give a complete picture of occupational morbidity in Russia and its structure. Therefore, a surveillance system should be created in Russia to provide the systematic collection, analysis, interpretation, and dissemination of morbidity data which documents labor conditions, various occupational hazards, and possible occupational disability. This mechanism of a a continuing surveillance system, when implemented, will be able to be used to predict the state of occupational health in the country, as well as in separate regions.
3. The expansion of the scientific basis of modern telemedical technologies, enabling greater transfer of medical information through telecommunication channels which will then increase the availability of qualified medical service for inhabitants of the distant regions of Russia.
During last several years, telemedical technologies have been actively developed in Russia. The technologies have allowed qualified medical services to be available for certain populations in a few regions of Russia, where such services had not been available otherwise.
Nevertheless, certain problems with telecommunications exist: legal and some organizational questions remain unclear; there is no standardized scientific method or basis for telemedical consults. Establishing a standard methodology, and addressing legal concerns will help expand the use of modern telemedical technologies, hastening their implementation in the sphere of occupational and environmental health.
1. http://www.who.int/health_topics/medical_informatics/en (last checked February 7, 2003).
2. E. Coiera, Guide to medical informatics, the Internet and telemedicine. Chapman & Hall, 1997.
3. R. Gibson Parrish II, S. M. McDonnell. Sources of health-related information, in: Principles and practice of public health surveillance. Ed. by S. M. Teutsch, R. E. Churchill, Oxford University Press, 2000.
4. Leigh JP, Markowitz SB, Fahs M et al. Occupational injury and illness in the United States. Estimates of costs, morbidity, and mortality. Arch Intern Med 1997 Jul 28;157(14):1557-68.
5. Occupational health. Recognizing and Preventing Work-Related Disease and Injury. Ed. by B. S. Levy, D. H. Wegman. Lippincott, Williams & Wilkins, 1999.
6. I. Yurgens. Reform of social insurance system. Nezavisimaya gazeta, June 26, 2001(in Russian).
7. N. F. Izmerov, E. I. Denisov. Methodology of occupational risk assessment in labor medicine. In: Social and hygienic monitoring – practice and scientific basis. Moscow, 2000. P. 181-186 (in Russian).
8. http://www.health.gov/environment/DefinitionsofEnvHealth/ehdef2.htm (last checked February 7, 2003)
9. Occupational diseases: Handbook. Ed. by N. F. Izmerov. Moscow, 1996 (in Russian)
10. O. Vasiliev, S. Stepanov. Federal register of occupational diseases is needed. Meditsinsky vestnik, September 26, 2002 (in Russian).
11. On occupational morbidity in Russian Federation in 2001. Report of Federal Center for State Sanitary and Epidemiological Control. Moscow, 2002 (in Russian).
12. http://www.safework.ru/RISOT/tables/T1.htm (last checked February 7, 2003, in Russian)
13. Workers Health Chartbook, 2000. NIOSH, 2000.
14. http://www.dadp.dgu.ru/NS.htm (last checked February 7, 2003, in Russian)
15. E. Vlasova. Reform of insurance. Nezavisimaya gazeta, April 4, 2001(in Russian).
16. http://www.depart.drugreg.ru/doc/p_334_99.html (last checked February 7, 2003, in Russian)
17. V. M. Cherepov, D. I. Timokhin, O.V. Klepikov, V. V. Zhukova. Methodical approaches to building information systems for social and hygienic monitoring. In: Social and hygienic monitoring – practice and scientific basis. Moscow, 2000. P. 14-19 (in Russian).
18. http://www.gsen.ru/soft/expsoft/krista/sgm.html (last checked February 7, 2003, in Russian)
19. N.V. Matveev. Contemporary communication technologies in hygiene and occupational health. In: Social and hygienic monitoring – practice and scientific basis. Moscow, 2000. P. 80-84 (in Russian).
20. N. B. Harmancioglu, O. Fistioglu, S. D. Ozkul, M. N. Alpaslan. Decision making in environmental management. In: Environmental data management. Kluwer Academic Publishers, 1998.
21. http://www.sra.org/ gloss3.htm#R (last checked February 7, 2003)
22. S. A. Melyuk, N. L. Karpov, N. A. Solonenko. Software and hardware for social and hygienic monitoring. In: Social and hygienic monitoring – practice and scientific basis. Moscow, 2000. P. 90-95. (in Russian).
23. N. A. Zabrodin, N. A. Kirianov, R. A. Kharten. Ranking the risk factors for population health. . In: Social and hygienic monitoring – practice and scientific basis. Moscow, 2000. P. 230-233. (in Russian).
24. V. F. Spirin, M. A. Mironenko, A. D. Doblo. Hygienic priorities social and hygienic monitoring in rural area. . In: Social and hygienic monitoring – practice and scientific basis. Moscow, 2000. P. 137-141. (in Russian).
25. Yu. P. Tikhomirov, M. P. Gracheva, I. V. Fedotova et al. On methodology of estimation of technogenic risk for female reproductive health. In: Ecological and environmental problems of population health preservation. Nizhny Novgorod, 1999 (in Russian).
26. http://www.fcgsen.ru (last checked February 7, 2003, in Russian)
27. A NIOSH look at data from the Bureau of Labor Statistics. NIOSH, 2000.
28. http://www.bls.gov/iif/home.htm#tables (last checked March 17, 2003)
29. ISA- The Swedish Information System for Occupational Accidents and Work-Related Diseases. SWEA Rapport 2000:16.
30. The information system for Occupational Injuries and the Work-related Health Problem Survey. Statistics Sweden 2002:2.
31. Bo Hagström. Svensk sjukvård i och under press. Studentlitteratur, Lund, 2002 (in Swedish).